Authors from the Netherlands and Canada have written a review on Non‐invasive ventilation (ventilators) used at night by people with COPD. The lead author, Tim Raveling, said “This review investigated if chronic non-invasive ventilation (NIV) is effective compared to standard care for patients with severe chronic obstructive pulmonary disease (COPD), using an analysis of pooled individual patient data. The results of this review on the patient centred outcomes indicates that reluctance towards the initiation of chronic NIV in stable hypercapnic COPD seems no longer warranted, whilst the application of chronic NIV after a severe COPD exacerbation can be discussed.”
The following is based on the plain language summary.
What is NIV?
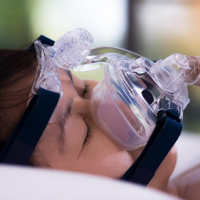
Non‐invasive ventilation (NIV) is a method to assist or replace spontaneous breathing (or normal breathing) with the aid of a machine called a ventilator, using a mask fitted over the nose or both the nose and mouth. NIV can be used chronically (long‐term) at the person's home if they have levels of carbon dioxide in their blood that are persistently too high.
What is the purpose of the review?
We wanted to discover if using chronic NIV at home during the night alongside standard therapy was better or worse than standard therapy alone in people with chronic obstructive pulmonary disease (COPD) who have raised carbon dioxide levels. In 2002 and 2013, we published our original Cochrane Reviews investigating this. It is important to check if new studies have been done that could be added to the existing studies of the original review and would change the findings.
What is individual participant data?
In this review we used individual participant data (IPD). This means that we attempted to collect original research data for each person who had participated in the original studies by requesting these individuals' data from the researcher who performed the study. We used IPD as this offers a greater chance to detect changes between groups of participants and enable the investigation of additional hypotheses. We used the IPD to perform our calculations.
Review question
What is the effect of chronic NIV in people with COPD on blood gases (oxygen and carbon dioxide), exercise capacity, quality of life, lung function, respiratory muscle function, COPD exacerbations and admissions, and survival?
What evidence did we find?
This review update identified 14 new studies in addition to those already in the review, so in total we included 21 studies. Ten of the studies looked at people in a stable phase (stable COPD) and four studies looked at people shortly after a COPD hospital admission (post‐exacerbation COPD). All studies included men and women. For our analyses, we used data from 778 people with stable COPD and 364 people with post‐exacerbation COPD. The evidence is current to 21 December 2020.
Results
In all people with COPD who had raised levels of carbon dioxide, chronic NIV for three and 12 months improved blood gases. In stable COPD, chronic NIV also might have improved quality of life, and survival seemed to be better compared to people who were treated with standard care only. There was no relevant benefit of NIV on exercise capacity. People using chronic NIV after a COPD admission experienced less benefit; carbon dioxide levels decreased, the time to the next hospital admission might have been longer when treated with NIV but quality of life and survival were not affected by chronic NIV.
Certainty of the results
Our confidence in the certainty (according to GRADE criteria) is good when looking at the blood gases. For the other outcomes, the certainty of the evidence is moderate to very low because the participants and the researcher were aware of the treatment the people received, and due to a wide range in the observed effect. This means that further research might change the results.
Read the full review here.
This summary was edited by Emma Dennett
